A tip of the hat to "PakMan" at PeakT for the reference to this article. The underlying work is on mice, but may have implications for humans.

 neurosciencenews.com
Original article:
neurosciencenews.com
Original article:
 doi.org
doi.org
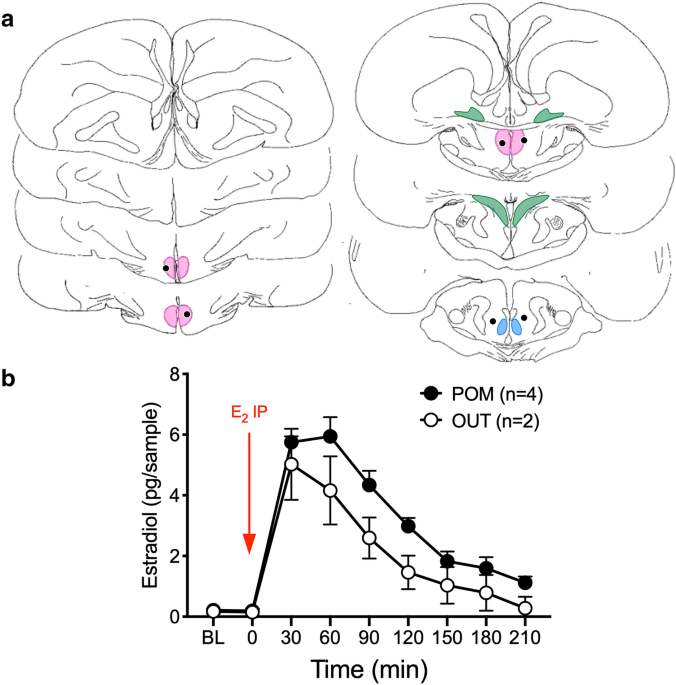
Summary: Researchers have uncovered specific regions of brain tissue where aromatase is present, that drives male sexual desire. Aromatase converts testosterone into estrogen in the brain, driving male sexual activity.
Source: Northwestern University
The locus of male sexual desire has been uncovered in specific regions of brain tissue where a key gene named aromatase is present, reports a new Northwestern Medicine study in mice.
The gene regulates sexual behavior in men, and thus can be targeted by drugs to either increase its function for low sexual desire or decrease its function for compulsive sexual desire, scientists said. Aromatase converts testosterone to estrogen in the brain, which drives male sexual activity.
The study was published Sept. 10 in the journal Endocrinology.
Aromatase’s full function in the adult brain had not previously been known.
“This is the first key finding to explain how testosterone stimulates sexual desire,” said senior author Dr. Serdar Bulun, chair of obstetrics and gynecology at Northwestern University Feinberg School of Medicine and Northwestern Medicine.
When Northwestern scientists knocked out aromatase selectively in the brain, sexual activity in male mice decreased by 50%, despite their having higher levels of blood testosterone levels (compared with control male mice).
...

Site of Male Sexual Desire Uncovered in Brain - Neuroscience News
Researchers have uncovered specific regions of brain tissue where aromatase is present, that drives male sexual desire. Aromatase converts testosterone into estrogen in the brain, driving male sexual activity.

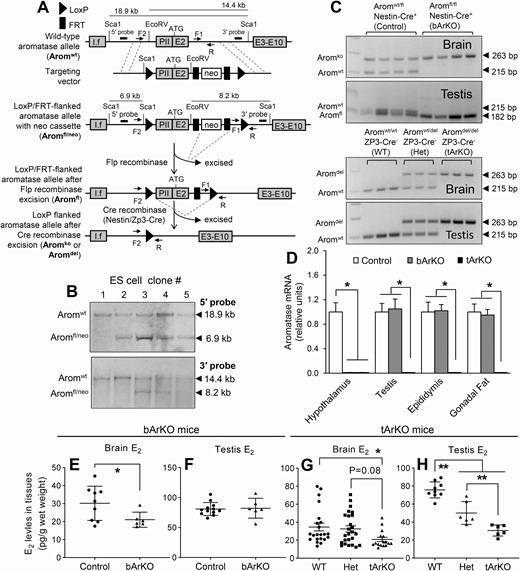
Brain Aromatase and the Regulation of Sexual Activity in Male Mice
Abstract. The biologically active estrogen estradiol has important roles in adult brain physiology and sexual behavior. A single gene, Cyp19a1, encodes aro
Last edited: