Most men who monitor their hormonal health are fixated on a single number: Total Testosterone. But for the symptomatic patient—the man struggling with unexplained fatigue, brain fog, or a vanishing libido despite "normal" lab results—that number is often a deception.
The problem lies in a massive "measurement gap." Think of Total Testosterone as a massive reservoir, but "Free Testosterone" (FT) as the only tap currently turned on. If the tap is clogged, the size of the reservoir doesn't matter. While clinicians have long suspected that Free Testosterone is the true "Gold Standard" for measuring androgen exposure, we have been remarkably poor at measuring it accurately—until now. A landmark study by Walravens et al. has just rewritten the manual, utilizing a rigorous analysis of 1,194 men to provide the most precise blueprint for male hormones ever published.
1. The "Free Hormone Hypothesis" and Why Total T is Often a Mirage
To understand why your lab report might be lying to you, you have to understand the "Free Hormone Hypothesis." In your bloodstream, the vast majority of testosterone is "handcuffed" to proteins—specifically Sex Hormone-Binding Globulin (SHBG) and albumin.The data reveals that a staggering 98% to 99% of your testosterone is bound and biologically "inert." Only the tiny 1% to 2% fraction that remains unbound is actually free to do the heavy lifting. As the study notes:
"According to the free hormone hypothesis, only this small, unbound, fraction is biologically active, being capable of crossing the cell membrane to exert its intracellular functions."
This makes Total Testosterone a frequent mirage, particularly in the context of obesity. Because weight gain causes SHBG levels to drop precipitously, a man's Total Testosterone may look alarmingly low—triggering a "false alarm" for hypogonadism—even if his biologically active Free Testosterone remains perfectly adequate. Conversely, a man with high SHBG might show a robust Total T score while his cells are actually starving for the hormone.
2. Your Lab’s "Calculated" Math Might Be 20% Off
In a revelation that should unsettle any clinical practitioner, the study highlights that most commercial labs don't actually measure your free testosterone. Instead, they use a mathematical shortcut called "Calculated Free Testosterone" (cFT), most commonly the Vermeulen formula.The verdict is in: when the researchers compared these math formulas against the actual gold-standard measurement—Equilibrium Dialysis followed by Liquid Chromatography-Tandem Mass Spectrometry (ED LC-MS/MS)—they found a consistent positive bias of approximately 20%.
This isn’t just a rounding error; it is an optimistic overestimation. Because these formulas typically skew high, thousands of symptomatic men are likely being told their levels are "normal" when their true, measured levels are significantly lower. The study makes a clear case: in a clinical environment where precision matters, mathematical approximations are a liability.
3. BMI: The Volume Knob on Male Androgens
While we know that excess weight impacts health, this study quantifies exactly how Body Mass Index (BMI) acts as a "volume knob," systematically turning down the body's androgen signals.Using restricted cubic spline regression, the researchers found that compared to a lean reference BMI of 22 kg/m²:
- A BMI of 30 (obesity) triggers a 14.4% drop in measured Free Testosterone (mFT).
- A BMI of 35 results in a 22.2% decrease.
4. The Aging Paradox: 76% of Older Men "Fail" Young Standards
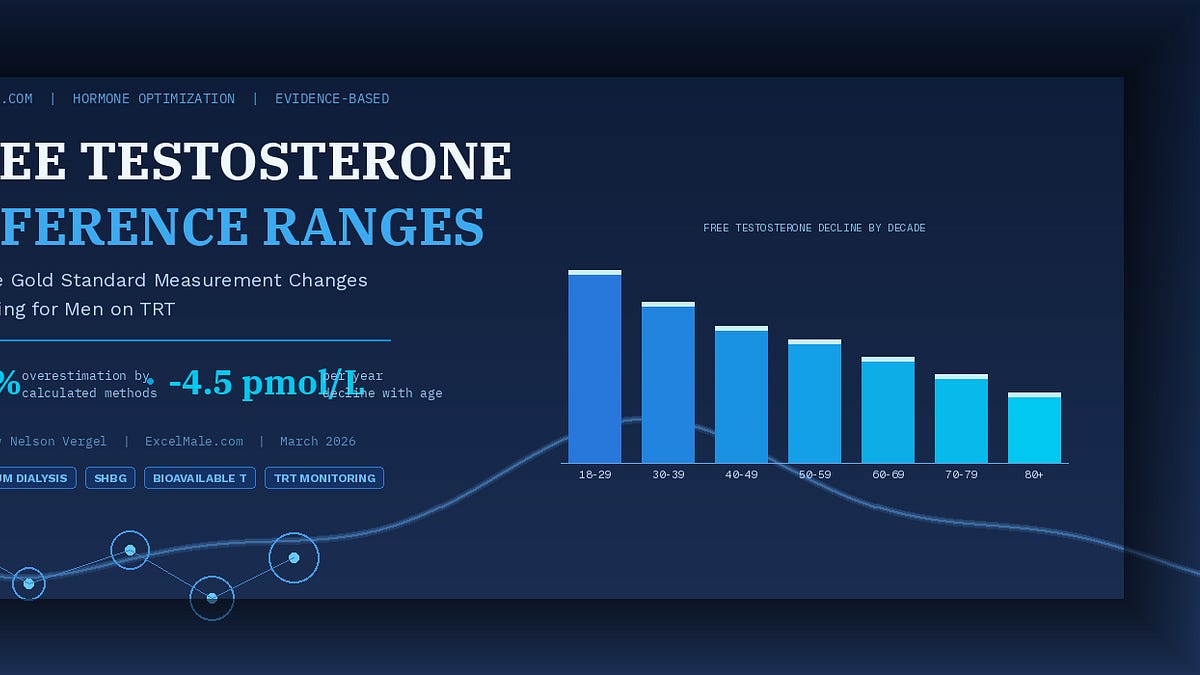
One of the most profound dilemmas in modern endocrinology is the "Aging Paradox." Should we judge an 80-year-old by the standard of a 20-year-old (the "T-score" approach), or should we accept a lower baseline as he ages (the "Z-score" approach)?The Walravens study provides a startling perspective: 76.3% of men aged 80 and older fall below the lower reference limit of men aged 18 to 39. To provide clarity, the researchers established new age-stratified ranges specifically for healthy, non-obese men:
- Ages 18–29: 239–877 pmol/L (approx. 6.9–25.3 ng/dL)
- Ages 80+: 49–250 pmol/L (approx. 1.4–7.2 ng/dL)
5. The "Wild West" of Global Testing Standards
The most troubling truth revealed by the study is that testosterone testing is currently a "Wild West." Because there is no universal reference measurement system, the lack of "harmonization" means your results are at the mercy of the lab you choose.The researchers noted that different laboratories can report mFT levels twice as high as others, even when testing identical populations. This lack of standardization is dangerous; a man could be diagnosed with hypogonadism at one lab and declared perfectly healthy at another.
The study issues a call to arms for the industry to adopt "IFCC-style" harmonization—similar to the global standards created for thyroid testing. Until we have a universal yardstick, a man’s hormonal diagnosis remains frustratingly subjective.
Conclusion: A New Blueprint for Men’s Health
As the largest study of its kind to employ the gold-standard Equilibrium Dialysis method, this research provides an essential correction to how we view male health. It proves that age and BMI are not just "lifestyle factors"—they are the primary architects of your hormonal profile.In an era moving toward personalized, precision medicine, we must move past the "reservoir" of Total Testosterone. If your health is ultimately defined by the hormones your body can actually use, the question you must ask your doctor is simple: Are you measuring what matters, or just what’s easy to calculate?
Comments from our in-house expert @madman
Largest dataset of mFT levels to date: male reference ranges spanning a wide age range, using a gold standard ED LC-MS/MS method - ExcelMale - #1 TRT & Testosterone Forum | Expert-Moderated Men's Health
Community
Last edited: