Check your estradiol (sensitive) blood levels cheaply: DiscountedLabs.com
REGISTERED MEMBERS: DOWNLOAD ATTACHED ESTRADIOL LECTURE HANDOUT AT THE BOTTOM OF THIS POST
Click here for a comprehensive article about the 18 things you should know about estradiol in men
By Nelson Vergel, BsChE, MBA
Note: This thread has 54 posts (3 pages).
Testosterone is the precursor hormone for estradiol. Estradiol is a hormone more abundant in women than men that are produced by the aromatization of testosterone in the liver, fat, and other cells. Nature created it for a reason. It has been shown to be responsible for healthy bone density but its role in men's sex drive, body composition, and other variables is a source of great debate.
When the HPT hormonal axis senses that testosterone or estradiol is high, it automatically decreases or shuts down testosterone production.
Many anti-aging or men's health clinics prescribe anastrozole, a blocker of estradiol production, to men who start testosterone replacement (TRT). Higher estradiol blood levels in the presence of low testosterone not only can cause breast tissue growth and possibly other issues. Some people speculate that high estradiol can also lead to erectile dysfunction but no scientific papers have been published on this subject. Since higher testosterone blood levels can originate higher estradiol levels, the belief is that using anastrozole will prevent breast tissue growth and erectile dysfunction by lowering any potential increase in estradiol. However, we have no data on how high is too high when it comes to this hormone in men using testosterone therapy. Some even speculate that low testosterone-to-estradiol ratios may be more closely correlated to gynecomastia and erectile problems than estradiol alone.
The truth about these speculations is starting to emerge but we still do not have enough data to say what the upper value of the optimal range of estradiol really is. We have a lot of evidence about the lower side of the optimal range since it has been found that estradiol blood levels below 10-20 pg/ml can increase bone loss in men. A recently published study also nicely demonstrated that low estradiol can be associated with higher fat mass and lower sexual function in men. So, be very careful when a clinic wants to put you on this drug without first justifying its use.
Another concerning fact is that many clinics may be using the wrong estradiol test that may overestimate the levels of this hormone in men. A sensitive estradiol test more accurately measures estradiol in men than the regular test, which costs less.
Sensitive Estradiol Blood Test: The Only Accurate Assay for Men
Fortunately, most men on TRT do not develop gynecomastia even without using anastrozole (gynecomastia is common in bodybuilders who may use high doses of testosterone, however). Those that have gynecomastia at TRT doses (100-200 mg of injectable testosterone or 5-10 grams of testosterone gel per day) may be genetically predisposed to having more aromatase activity or have liver dysfunction. Treating all men who start TRT with anastrozole from the start may be counterproductive since this may lower estradiol to very low levels. Some physicians monitor estradiol blood levels after 6-8 weeks of having a man start TRT alone using the ultrasensitive estradiol test to determine if anastrozole use is warranted. Doses range from 0.25 mg per week to some clinics using excessive doses of 1 mg three times per week. After 4-6 weeks on anastrozole, its dose can be adjusted to ensure than estradiol is not under 20 pg/ml. Fortunately, many men on TRT do not need anastrozole at all.
What to Do if You Crashed Your Estradiol?
Treatment of estrogen (estradiol) levels in men on TRT: An anonymous doctor survey

 www.excelmale.com
www.excelmale.com


 www.excelmale.com
www.excelmale.com
My opinion is that:
1- AIs should not be prescribed at TRT start.
2- Sensitive estradiol should be measured after 6-8 weeks
3- A ratio of testosterone to estradiol of 14 and higher is not a cause of gynecomastia (divide ng/dL by pg/mL). All men on TRT have that kind of ratios.
4- Unless you have strong genetic predisposition to gynecomastia, AI's should not be used. If AIs are used, most men do not need doses over 0.25- 0.5 mg per week.
5- Water retention and sensitive nipples are usually NOT a symptom of high estradiol.
6- Using AIs have never been proven to decrease water retention. Water retention on TRT is caused by sodium retention.
7- It is not easy to recover from crashing your estradiol. Low estradiol can decrease sex drive and penis sensitivity, bone density and increase fat mass.
Why is estradiol important for men?
One of the most common problems reported on ExcelMale: I crashed my estradiol
More articles on estradiol in men: Click here
Estradiol in Men: Impact on Cognitive Function and Heart Disease during Testosterone Therapy | Discounted Labs
Estradiol in Men on TRT: Impact on Brain and Heart
Estradiol's Role in Men's Health: Top 18 Facts
Estradiol Blood Level in Men: Why It is Important
Is Estradiol a Friend or Enemy of Men?
Men’s Heart Disease Partly Due to Low Estrogen





 www.excelmale.com
www.excelmale.com

 www.excelmale.com
www.excelmale.com

 www.excelmale.com
www.excelmale.com

 www.excelmale.com
www.excelmale.com
REGISTERED MEMBERS: DOWNLOAD ATTACHED ESTRADIOL LECTURE HANDOUT AT THE BOTTOM OF THIS POST
Click here for a comprehensive article about the 18 things you should know about estradiol in men
By Nelson Vergel, BsChE, MBA
Note: This thread has 54 posts (3 pages).
Testosterone is the precursor hormone for estradiol. Estradiol is a hormone more abundant in women than men that are produced by the aromatization of testosterone in the liver, fat, and other cells. Nature created it for a reason. It has been shown to be responsible for healthy bone density but its role in men's sex drive, body composition, and other variables is a source of great debate.
When the HPT hormonal axis senses that testosterone or estradiol is high, it automatically decreases or shuts down testosterone production.
Many anti-aging or men's health clinics prescribe anastrozole, a blocker of estradiol production, to men who start testosterone replacement (TRT). Higher estradiol blood levels in the presence of low testosterone not only can cause breast tissue growth and possibly other issues. Some people speculate that high estradiol can also lead to erectile dysfunction but no scientific papers have been published on this subject. Since higher testosterone blood levels can originate higher estradiol levels, the belief is that using anastrozole will prevent breast tissue growth and erectile dysfunction by lowering any potential increase in estradiol. However, we have no data on how high is too high when it comes to this hormone in men using testosterone therapy. Some even speculate that low testosterone-to-estradiol ratios may be more closely correlated to gynecomastia and erectile problems than estradiol alone.
The truth about these speculations is starting to emerge but we still do not have enough data to say what the upper value of the optimal range of estradiol really is. We have a lot of evidence about the lower side of the optimal range since it has been found that estradiol blood levels below 10-20 pg/ml can increase bone loss in men. A recently published study also nicely demonstrated that low estradiol can be associated with higher fat mass and lower sexual function in men. So, be very careful when a clinic wants to put you on this drug without first justifying its use.
Another concerning fact is that many clinics may be using the wrong estradiol test that may overestimate the levels of this hormone in men. A sensitive estradiol test more accurately measures estradiol in men than the regular test, which costs less.
Sensitive Estradiol Blood Test: The Only Accurate Assay for Men
Fortunately, most men on TRT do not develop gynecomastia even without using anastrozole (gynecomastia is common in bodybuilders who may use high doses of testosterone, however). Those that have gynecomastia at TRT doses (100-200 mg of injectable testosterone or 5-10 grams of testosterone gel per day) may be genetically predisposed to having more aromatase activity or have liver dysfunction. Treating all men who start TRT with anastrozole from the start may be counterproductive since this may lower estradiol to very low levels. Some physicians monitor estradiol blood levels after 6-8 weeks of having a man start TRT alone using the ultrasensitive estradiol test to determine if anastrozole use is warranted. Doses range from 0.25 mg per week to some clinics using excessive doses of 1 mg three times per week. After 4-6 weeks on anastrozole, its dose can be adjusted to ensure than estradiol is not under 20 pg/ml. Fortunately, many men on TRT do not need anastrozole at all.
What to Do if You Crashed Your Estradiol?
Treatment of estrogen (estradiol) levels in men on TRT: An anonymous doctor survey
Estradiol is an Important Hormone for Men - Excel Male TRT Forum
* read full paper (pdf) MECHANISMS IN ENDOCRINOLOGY Estradiol as a male hormone Nicholas Russell and Mathis Grossmann Abstract Evidence has been accumulating that, in men, some of the biological actions traditionally attributed to testosterone acting via the androgen receptor may...
Estrogen is Essential for Muscle Growth in Bodybuilders - Excel Male TRT Forum
William Llewellyn’s, ANABOLICS Estrogen Aromatization Testosterone is the primary substrate used in the male body for the synthesis of estrogen (estradiol), the principal female sex hormone. Although the presence of estrogen may seem quite unusual in men, it is structurally very similar to...
My opinion is that:
1- AIs should not be prescribed at TRT start.
2- Sensitive estradiol should be measured after 6-8 weeks
3- A ratio of testosterone to estradiol of 14 and higher is not a cause of gynecomastia (divide ng/dL by pg/mL). All men on TRT have that kind of ratios.
4- Unless you have strong genetic predisposition to gynecomastia, AI's should not be used. If AIs are used, most men do not need doses over 0.25- 0.5 mg per week.
5- Water retention and sensitive nipples are usually NOT a symptom of high estradiol.
6- Using AIs have never been proven to decrease water retention. Water retention on TRT is caused by sodium retention.
7- It is not easy to recover from crashing your estradiol. Low estradiol can decrease sex drive and penis sensitivity, bone density and increase fat mass.
Why is estradiol important for men?
One of the most common problems reported on ExcelMale: I crashed my estradiol
More articles on estradiol in men: Click here
Estradiol in Men: Impact on Cognitive Function and Heart Disease during Testosterone Therapy | Discounted Labs
Estradiol in Men on TRT: Impact on Brain and Heart
Estradiol's Role in Men's Health: Top 18 Facts
Estradiol Blood Level in Men: Why It is Important
Is Estradiol a Friend or Enemy of Men?
Men’s Heart Disease Partly Due to Low Estrogen
How to Predict Estradiol and DHT at Different Testosterone Doses - Excel Male TRT Forum
I was able to come up with a table using the predictive model equation derived from data in this study: The Effects of Injected Testosterone Dose and Age on the Conversion of Testosterone to Estradiol and Dihydrotestosterone in Young and Older Men Summary This video discusses a research paper...
Estradiol is an Important Hormone for Men - Excel Male TRT Forum
* read full paper (pdf) MECHANISMS IN ENDOCRINOLOGY Estradiol as a male hormone Nicholas Russell and Mathis Grossmann Abstract Evidence has been accumulating that, in men, some of the biological actions traditionally attributed to testosterone acting via the androgen receptor may...
Estradiol in Men: Libido and Brain Function - Excel Male TRT Forum
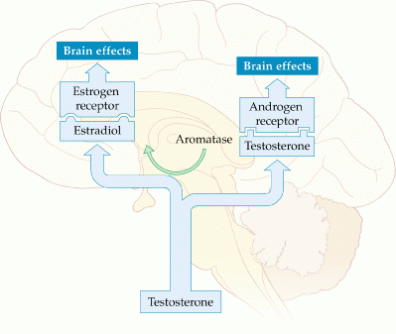
Role of estradiol in the brain The effect of estradiol on libido is seen at various levels of regulation, starting with direct effects in the brain (Figure 1). Areas of the brain that control sexual behavior in mammals are thought to do so via pheromones that induce specific sexual effects on...
Testosterone Needs to Be Converted into Estradiol to Prevent Fat Accumulation - Excel Male TRT Forum
How Targeting Fat Cells’ Estrogen Receptors Could Fight Obesity Tracy Hampton, PhD In adipocytes, fat cells, a particular estrogen-receptor appears critical for energy supplying mitochondria to function properly. The discovery points to a potential drug target for boosting fat tissue...
Last edited: