Nelson Vergel
Founder, ExcelMale.com
Most absorption of testosterone in testosterone gels happens during the first 4 hours. The 1.62 % Androgel package insert says this about showering after testosterone gel application and using moisturizers/sun block:
"Effect of showering
In a randomized, 3-way (3 treatment periods without washout period) crossover study in 24 hypogonadal men, the effect of showering on testosterone exposure was assessed after once daily application of AndroGel 1.62% 81 mg to upper arms/shoulders for 7 days in each treatment period. On the 7th day of each treatment period, hypogonadal men took a shower with soap and water at either 2, 6, or 10 hours after drug application. The effect of showering at 2 or 6 hours post-dose on Day 7 resulted in 13% and 12% decreases in mean Cavg, respectively, compared to Day 6 when no shower was taken after drug application.
Showering at 10 hours after drug application had no effect on bioavailability. The amount of testosterone remaining in the outer layers of the skin at the application site on the 7th day was assessed using a tape stripping procedure and was reduced by at least 80% after showering 2-10 hours post-dose compared to on the 6th day when no shower was taken after drug application.
Effect of sunscreen or moisturizing lotion on absorption of testosterone
In a randomized, 3-way (3 treatment periods without washout period) crossover study in 18 hypogonadal males, the effect of applying a moisturizing lotion or a sunscreen on the absorption of testosterone was evaluated with the upper arms/shoulders as application sites. For 7 days, moisturizing lotion or sunscreen (SPF 50) was applied daily to the AndroGel 1.62% application site 1 hour after the application of AndroGel 1.62% 40.5 mg. Application of moisturizing lotion increased mean testosterone Cavg and Cmax by 14% and 17%, respectively, compared to AndroGel 1.62% administered alone. Application of sunscreen increased mean testosterone Cavg and Cmax by 8% and 13%, respectively, compared to AndroGel 1.62% applied alone. "
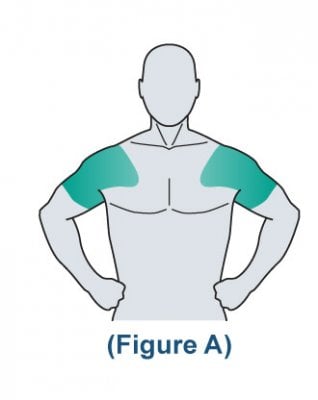
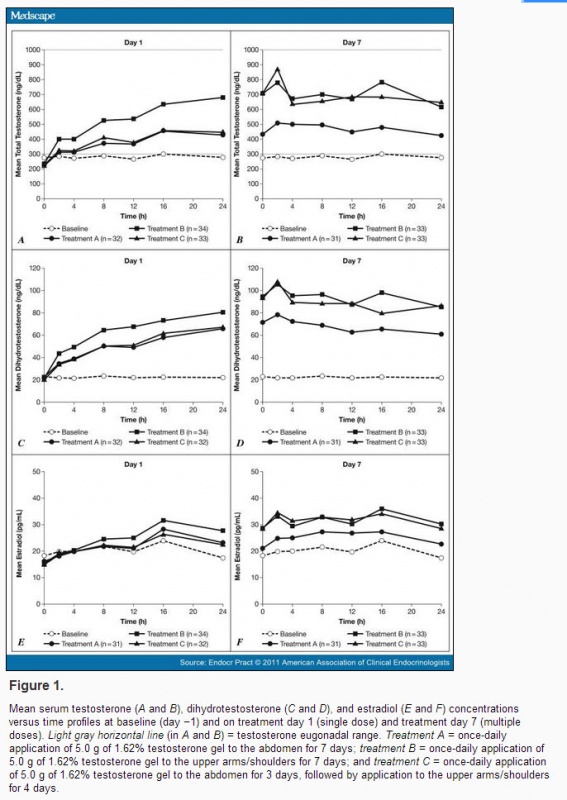
This graph shows how applying on shoulders (treatment B) gets blood levels of testosterone higher than applying testosterone gel on abdominal area (treatment A). It is probably related to the lower amount of fat in the shoulders that makes it easier for testosterone to get to the blood stream.
Message:
1- Applying on shoulders gets more testosterone absorbed by abdominals.
2- Showering or sweating after 4 hours is OK.
3- Using moisturizers or sunblock after applying testosterone gels increases absorption by 8-13 percent.
"Effect of showering
In a randomized, 3-way (3 treatment periods without washout period) crossover study in 24 hypogonadal men, the effect of showering on testosterone exposure was assessed after once daily application of AndroGel 1.62% 81 mg to upper arms/shoulders for 7 days in each treatment period. On the 7th day of each treatment period, hypogonadal men took a shower with soap and water at either 2, 6, or 10 hours after drug application. The effect of showering at 2 or 6 hours post-dose on Day 7 resulted in 13% and 12% decreases in mean Cavg, respectively, compared to Day 6 when no shower was taken after drug application.
Showering at 10 hours after drug application had no effect on bioavailability. The amount of testosterone remaining in the outer layers of the skin at the application site on the 7th day was assessed using a tape stripping procedure and was reduced by at least 80% after showering 2-10 hours post-dose compared to on the 6th day when no shower was taken after drug application.
Effect of sunscreen or moisturizing lotion on absorption of testosterone
In a randomized, 3-way (3 treatment periods without washout period) crossover study in 18 hypogonadal males, the effect of applying a moisturizing lotion or a sunscreen on the absorption of testosterone was evaluated with the upper arms/shoulders as application sites. For 7 days, moisturizing lotion or sunscreen (SPF 50) was applied daily to the AndroGel 1.62% application site 1 hour after the application of AndroGel 1.62% 40.5 mg. Application of moisturizing lotion increased mean testosterone Cavg and Cmax by 14% and 17%, respectively, compared to AndroGel 1.62% administered alone. Application of sunscreen increased mean testosterone Cavg and Cmax by 8% and 13%, respectively, compared to AndroGel 1.62% applied alone. "
This graph shows how applying on shoulders (treatment B) gets blood levels of testosterone higher than applying testosterone gel on abdominal area (treatment A). It is probably related to the lower amount of fat in the shoulders that makes it easier for testosterone to get to the blood stream.
Message:
1- Applying on shoulders gets more testosterone absorbed by abdominals.
2- Showering or sweating after 4 hours is OK.
3- Using moisturizers or sunblock after applying testosterone gels increases absorption by 8-13 percent.

Last edited:

















