Dr Justin Saya MD
Moderator
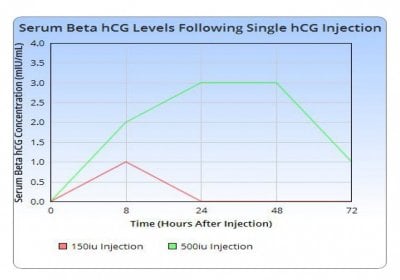
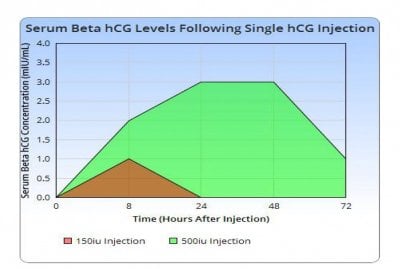
Community - I am sharing and have attached the write-up of a recent small case study I have conducted on quantitative serum beta hCG concentrations relating to hCG injections. This study is limited to dosages of 150iu and 500iu, although I hope to obtain more data in the near future.
P.S. Attempted to copy/paste plain text for those that may have a challenge viewing the pdf on mobile, but formatting wouldn't cooperate.
P.S. Attempted to copy/paste plain text for those that may have a challenge viewing the pdf on mobile, but formatting wouldn't cooperate.
Attachments
Last edited by a moderator: